The dislocation or subluxation of IOLs has been an uncommon but recurrent complication throughout the history of their implantation. If the IOL is subluxated but still stable within the anterior segment, the surgeon may use an anterior approach to fixate the implant. If the IOL is unstable or dislocated posteriorly into the vitreous cavity, he should approach and retrieve the IOL via the posterior segment or pars plana vitrectomy and then reposition, exchange, or remove the lens.1-7
The Approach
With IOLs that are unstable or posteriorly dislocated into the vitreous cavity, the advantages of a pars plana surgical approach include (1) a closed system with continuous infusion that allows precise maneuvers in a controlled surgical environment, (2) the clear visualization of surgical maneuvers through an undistorted cornea, and (3) bimanual manipulation of the unstable, dislocated implant. In addition, the surgeon can support the dislocated IOL from a posterior-to-anterior direction by passing instruments through the pars plana (Figure 1) as opposed to using a limbal or clear corneal approach, which requires passing instruments in an anterior-to-posterior direction to manipulate the dislocated IOL. Although improved techniques and instrumentation have greatly facilitated the management of these cases, new IOL designs and presentations such as in-the-bag IOL dislocations (where the IOL is encased within the capsular bag and dislocated due to zonular dehiscence8,9) present new challenges in management.
HOW TO PROCEED
The decision to remove, exchange, or reposition the IOL depends on the clinical situation. It is advisable to remove the lens in eyes with a poor visual prognosis, associated complicated retinal pathology such as retinal detachment, or damaged IOLs.1-3 Exchanging the IOL for either a flexible-loop ACIOL or a sclerally fixated PCIOL is a reasonable management option, but it has the disadvantage of creating a large wound in the anterior segment for the removal of the dislocated IOL and the implantation of a new one.1-3,7
Repositioning the dislocated IOL reuses the original IOL, the refractive power of which provided functional vision prior to dislocation, and avoids the need for a large wound in the anterior segment.1-7 Difficulties in manipulating the unstable dislocated IOL and trying to loop sutures around it have led some surgeons to abandon repositioning procedures, however. Moreover, a comparative, multisurgeon series found no difference in visual outcomes after the repositioning of the dislocated IOL versus its exchange for an ACIOL.7
REPOSITIONING DISLOCATED IOLs
Background
Manipulating an unstable, dislocated IOL in the vitreous cavity is technically difficult. For that reason, surgeons have developed many techniques to reposition and, if necessary, sclerally fixate a PCIOL’s haptics.1-6 Ideally, there is an intact rim of peripheral capsule over which the surgeon can reposition the IOL and its supporting haptics, thus minimizing surgical trauma and allowing the quickest recovery of vision. If the dislocation occurs many years after the IOL’s initial implantation even if there is a residual capsular rim, however, I have found that either the capsular-zonular support system has become incapable of supporting the IOL’s haptics long-term, or the original IOL’s haptics are too flexible or are inadequate to prevent repeat dislocation over time. In cases of late, recurrent dislocation, the surgeon should place at least one scleral-fixation suture.
If the capsular support for the haptics is inadequate, the surgeon may reposition dislocated PCIOLs with scleral-fixation sutures. With adequate capsular support for one haptic (at least 5 clock hours), he may use scleral fixation for one haptic and the residual capsule for the other haptic.4,5 If there is inadequate capsular support for one haptic, then I prefer to remove the residual capsule during the pars plana vitrectomy and sclerally fixate both haptics. In order to evaluate and plan for the surgical procedure, it is important to conduct a careful, tangential, slit-lamp examination for residual capsular support during the preoperative examination.
Creating the Suture Loop for Scleral Fixation
There are several techniques for looping a suture around the haptic of a dislocated IOL in eyes with inadequate residual capsular support.1-6 Internal looping techniques are too numerous to describe in depth in this article, but they include multiple passes of the needle around the haptic through sclerotomies or paracentesis sites, looping the haptic with a threaded needle or a loop passed through a needle, holding a suture loop with a forceps, or lassoing the haptic with a pretied loop or slipknot.1-3 These techniques work well if the IOL is relatively stable in a position posterior to the pupil so that it does not fall posteriorly during looping maneuvers. These intraocular maneuvers can be cumbersome and frustrating, however, when the dislocated IOL is unstable and mobile in the vitreous cavity, especially following pars plana vitrectomy.
Haptic Externalization
A technique called haptic externalization allows the surgeon to securely place the scleral-fixation suture prior to reimplantating an IOL into the eye. It also stabilizes the previously unstable IOL and thus makes further manipulation safer and more controlled.4-6 Clement Chan, MD, first described haptic externalization through a pars plicata fixation sclerotomy.6 Once the surgeon externalizes the haptic, he tightens the suture loop down around the haptic and reimplants it.
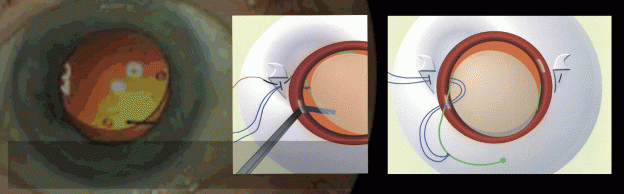
In order to stabilize dislocated IOLs, I developed a technique of bringing the dislocated PCIOL back into the anterior chamber and then externalizing the haptic through a clear corneal incision (Figure 2). After I fixate the suture to the haptic outside the eye, I pass the suture posteriorly through the clear corneal incision, through the pupil, and posterior to the iris, where I retrieve it through a fixation sclerotomy, 1.25mm posterior to the limbus (Figure 3). The implant is then in its usual position, and I can reimplant it in a controlled fashion. The clear corneal externalization allows me direct visualization of the haptic externalization and thus minimizes the risk of damage to the haptic during externalization.
One important hint for performing an externalization technique is to grasp the tip of the haptic and to follow its curve during externalization to prevent breaking or bending the haptic.
In-the-Bag IOL Dislocations
Managing in-the-bag dislocation of an IOL is especially challenging, because the haptics are enmeshed within the residual capsule and lens debris. Although the highest incidence of this complication has been reported with pseudoexfoliation,8,9 it can also occur with uveitis and trauma or without an identifiable cause.9 If the complex is still relatively stable within the anterior segment, the surgeon may grasp and remove the entire complex through an anterior segment wound. In addition, some surgeons have found posterior-assisted levitation10 with viscoelastic to be a useful approach that floats the complex anteriorly in order to allow its removal from this direction. Suturing through the capsular bag is another alternative for achieving scleral fixation. “Cheesewiring” the suture loop through the residual capsule as well as inadequate long-term stability of the suture loops around the haptics through the capsule may be a risk for future redislocation, however.11
Presently, if an IOL in the bag dislocates into the vitreous cavity, I prefer to (1) use a posterior segment approach with vitrectomy, (2) stabilize the IOL-capsular bag complex with a forceps, and (3) dissect the residual capsule and lens debris off the haptics and possibly the optic of the dislocated IOL. I may then externalize and fixate the haptics to the sclera by tightening the suture loops directly onto the haptic in order to minimize the IOL’s future redislocation.9,11
Gregg T. Kokame, MD, is Medical Director of The Retina Center at Pali Momi and is Clinical Professor, Division of Ophthalmology, Department of Surgery, the University of Hawaii School of Medicine, Honolulu. He states that he holds no financial interest in any product, technology, or company mentioned herein. Dr. Kokame may be reached at (808) 487-8928; retinahi@aol.com.
- Mello MO, Scott IU, Smiddy WE, et al. Surgical management and outcomes of dislocated intraocular lenses. Ophthalmology. 2000;107:62-67.
- Chan CK, Agarwal A, Agarwal S, Agarwal A. Management of dislocated intraocular implants. Ophthalmol Clin North Am. 2001;14:681-693.
- Smiddy WE, Ibanez GV, Alfonso E, Flynn HW Jr. Surgical management of dislocated intraocular lenses. J Cataract Refract Surg. 1995;21:64-69.
- Kokame GT, Yamamoto I, Mandel H. Scleral fixation of dislocated posterior chamber intraocular lenses. Temporary haptic externalization through a clear corneal incision. J Cataract Refract Surg. 2004;30:1049-1056.
- Kokame GT, Atebara NH, Bennett MD. Modified technique of haptic externalization for scleral fixation of posterior chamber implants. Am J Ophthalmol. 2001;131:129-131.
- Chan CK. An improved technique for management of dislocated posterior chamber implants. Ophthalmology. 1992;99:51-57.
- Sarrafizadeh R, Ruby AJ, Hassan TS, et al. A comparison of visual results and complications in eyes with posterior chamber intraocular lens dislocation treated with pars plana vitrectomy and lens repositioning or lens exchange. Ophthalmology. 2001;108:82-89.
- Jehan FS, Mamalis N, Crandall AS. Spontaneous late dislocation of intraocular lens within the capsular bag in pseudoexfoliation patients. Ophthalmology. 2001;108:1727-1731.
- Gross JG, Kokame GT, Weinberg DV. The Dislocated In-The-Bag Intraocular Lens Study Group. In-the-bag intraocular lens dislocation. Am J Ophthalmol. 2004;137:630-635.
- Chang DF. Viscoelastic levitation of posteriorly dislocated intraocular lenses from the anterior vitreous. J Cataract Refract Surg. 2002;28:1515-1519.
- Kokame GT, Gross JG, Weinberg DV. The Dislocated In-the-Bag Intraocular Lens Study Group. In-the-bag intraocular lens dislocation. Author Reply. Am J Ophthalmol. 2005;139:953-954.

No comments yet.